-
Men's Health
-
Women's Health
-
Sexual Health
-
Chronic
-
Travel
-
Book online for vaccinations for
travel and general health in one
of over 60 clinics nationwide
-
-
Wellbeing
-
Testing Services
-
Help & Contact
-
What Is Superdrug Online Doctor?
We're a service that helps you order treatments online from UK-registered doctors with free, discreet, to-your-door deliveries.
-

Did Lockdowns Lead to Less STIs?
Key Takeaways
- STI infections decreased by 32% during the COVID-19 lockdowns.
- Online searches for STIs and at-home tests spiked during the March 2020 lockdown.
- Video and online health appointments rose by 61% in September 2020.
- Individuals whose partners tested positive for an STI were less likely to get tested themselves during the pandemic.
In its latest Global Progress Report, the World Health Organisation highlighted the global progress being made in reducing the number of HIV and STI cases but noted that most targets have not been reached. The COVID-19 pandemic placed greater strain on many health services, threatening to halt or reverse global progress thus far. According to Public Health England, the country experienced a reduction in sexual health and HIV consultations, tests, and vaccinations during 2020.
We wanted to further explore how the COVID-19 pandemic impacted STI testing and diagnosis. Did lockdowns and social distancing reduce the spread of STIs? Were people afraid to get the necessary testing and treatment for STIs during the pandemic? Did people that tested positive for an STI inform their partner, and how likely were they to have transmitted the infection to others?
To answer questions like these, we first extracted transmission data from Public Health England reports for 2016 to 2020 to see if there were any trends in the rate of chlamydia, gonorrhoea, syphilis, and HIV during the pandemic. We then looked at how the pandemic affected the ways in which people sought STI testing and treatment. To reduce the spread of COVID-19, many doctors transitioned to telehealth platforms; consequently, we asked for respondents' thoughts on discussing their sexual health online versus in person. Read on to see what we discovered.
Infection Rates in the UK
Public Health England tracks rates of STIs throughout the region. Below you'll find the number of cases for four of the best-known STIs from 2016 to 2020, both overall and according to gender.
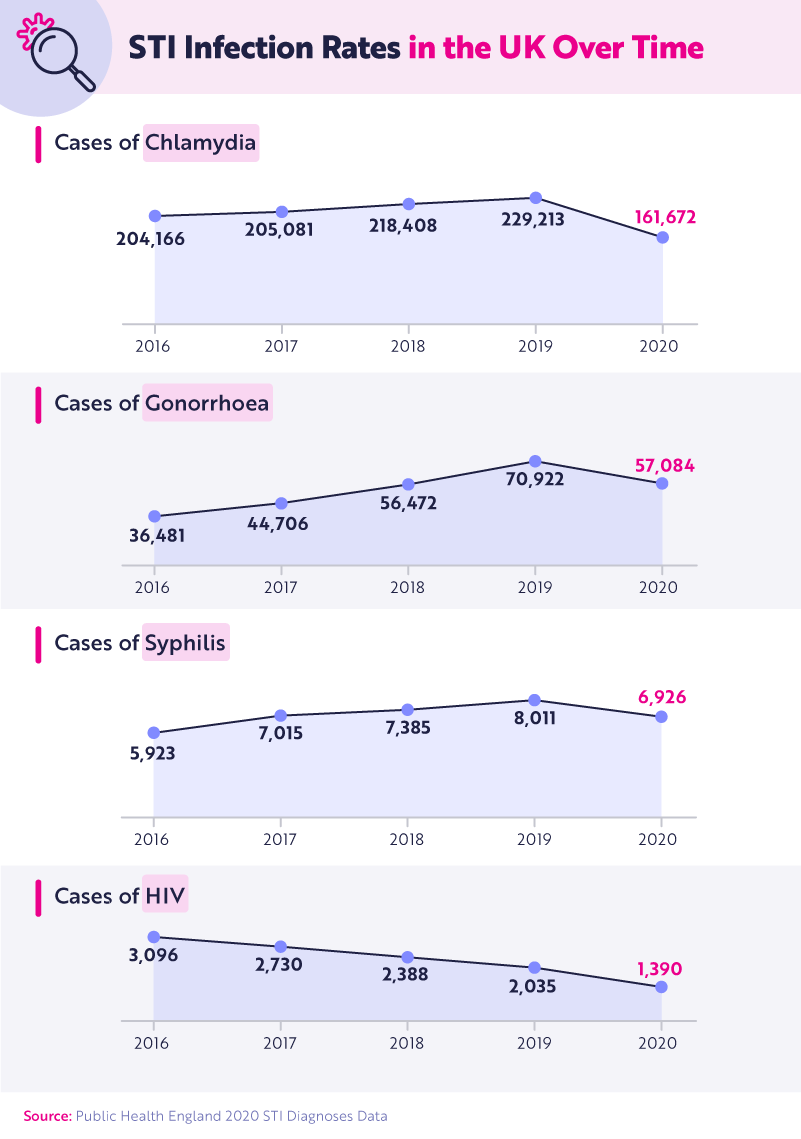
Since 2016, cases of chlamydia, gonorrhoea, and syphilis all increased year over year until 2020, when infection rates rapidly declined—perhaps as a result of COVID-19 restrictions making it difficult to meet new sexual partners. 2020 has been called the "lost year" and the "year of celibacy" by singles, many of which said they wouldn't be comfortable going home with a partner until all restrictions were lifted.
STI cases vary by gender. For instance, in the UK men are more likely to contract gonorrhoea, syphilis, and HIV, while women generally have a higher instance of chlamydia. Recently, the National Health Service (NHS) decided to focus its chlamydia screening efforts on women, who are more susceptible to serious consequences from chlamydia. Syphilis has also been increasing the most among men who have sex with other men, who accounted for 78% of new diagnoses in the UK in 2017.Experts say this rise may be due to apps like Grindr, which make casual sex more available. This would also help explain the decrease in cases in 2020 when people were more reluctant to take online encounters offline.
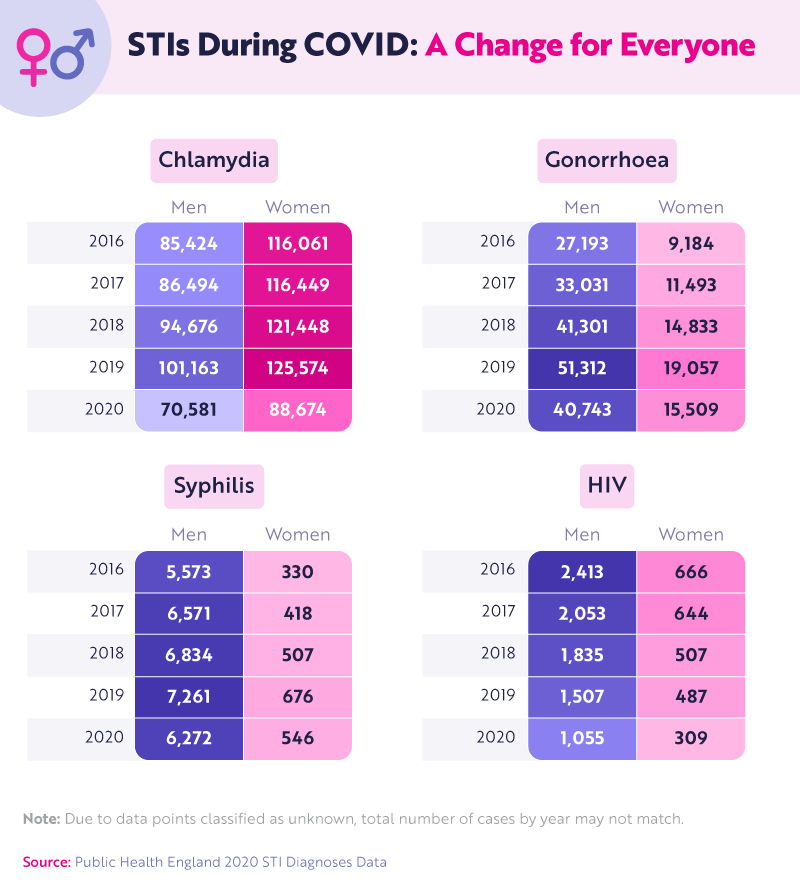
HIV is the only STI that was on a downward trend before the COVID-19 pandemic, in large part due to the efficacy of PrEP, or pre-exposure prophylaxis, where medications are used to help prevent the spread of HIV. Public Health England launched the PrEP IMPACT trial in 2017 and has since found that gay and bisexual men who enrolled in the trial had 87% fewer HIV infections than those who did not use PrEP.
But PrEP may only be half of the story. While HIV had been trending down since 2016, with cases falling 13%, on average, between 2016 and 2019, infection rates dropped almost twice as much in 2020, falling 32%. This suggests it could be the combination of PrEP and COVID social contact restrictions that made such a strong positive impact on reducing the spread of HIV. Less people visiting sexual health clinics and doing HIV tests could also have had a role to play in making HIV diagnosis rates lower during the pandemic.
Getting Tested During Lockdown
Given the changes in STI cases during the pandemic, we wanted to find out how people's behaviour around STIs changed during the pandemic. Were they still concerned about contracting STIs? And if so, where did they go for testing and treatment?
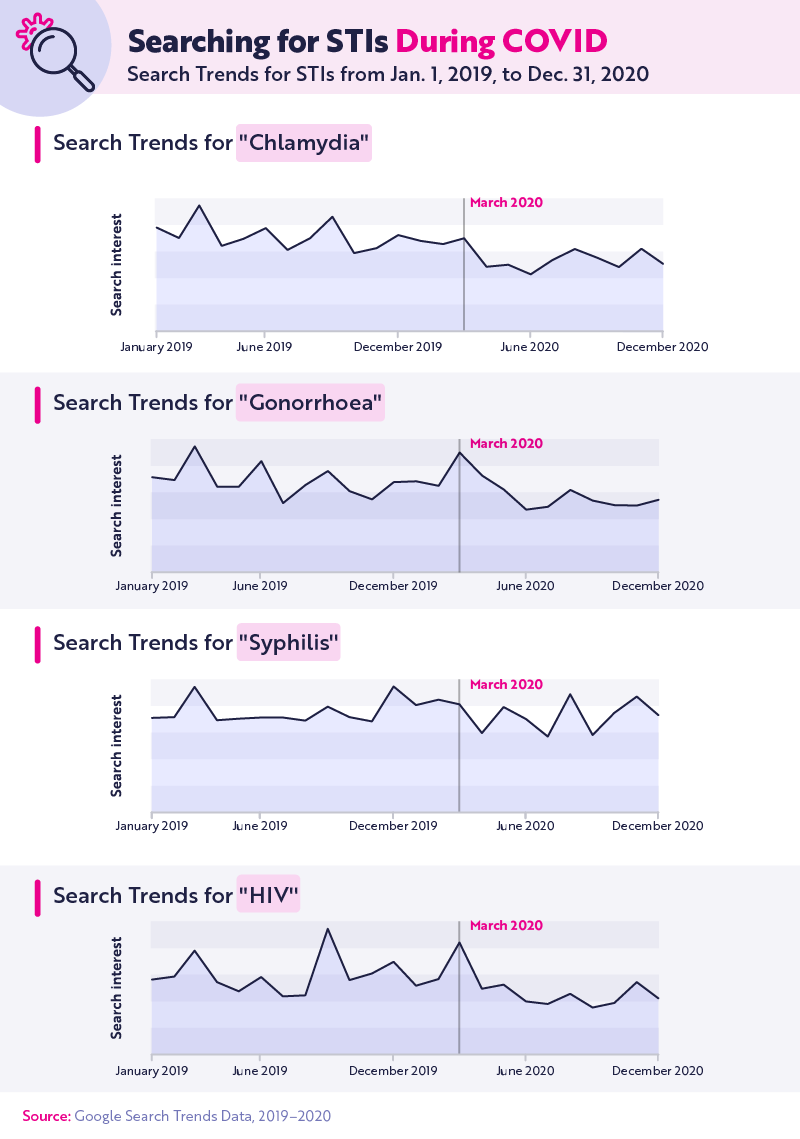
We examined Google search trends from the UK to see if people were researching STIs at home. The results show a spike in searches for chlamydia, gonorrhoea, and HIV at the height of pandemic lockdowns in March 2020. Searches for "home chlamydia test nhs" alone increased 300% during this time period. UK sexual health services rose to the challenge by ramping up their online and phone services during COVID.
Experts were optimistic and said that if everyone would get tested and treated while at home during lockdown, nationwide STI numbers could dramatically be reduced.
STI Treatment During Lockdown
With 54% of UK sites for sexual health services closed during the pandemic, residents who thought they may have an STI were left to seek out testing, diagnosis, and possibly even treatment online or over the phone. We dug into how respondents felt about getting sexual health treatment online versus in person.
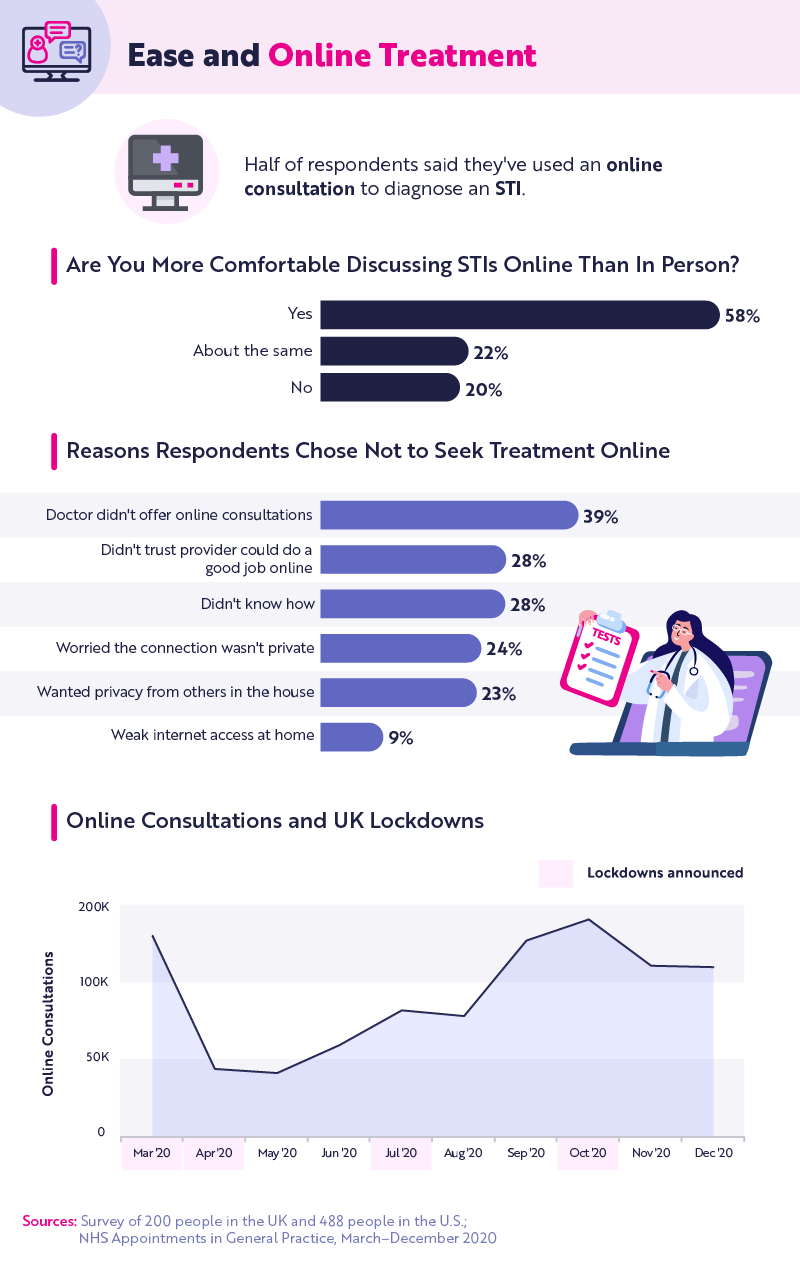
Half of respondents said they've used an online service to diagnose an STI. In fact, 58% of respondents indicated they'd prefer to talk about STIs online rather than in person. Despite this, the online appointments still remain a small fraction of total GP visits in 2020. Online visits represented only about 0.3% to 0.5% of total GP visits from March through December 2020 compared to face-to-face visits, which accounted for about half of GP visits during that time. In fact, there was a sharp decline in online appointments from April through August of 2020, and they didn't start to pick up again until September 2020 when there was a 61% increase in video and online appointments. We may continue to see more online and virtual health visits as the UK gets acclimated to telemedicine after the rush to adapt during the pandemic.
Making the Call
After researching case data for the four aforementioned STIs, we gathered information about partner notification from 2016 to 2020. Once notified of potential exposure, how many got tested, and what were the results?
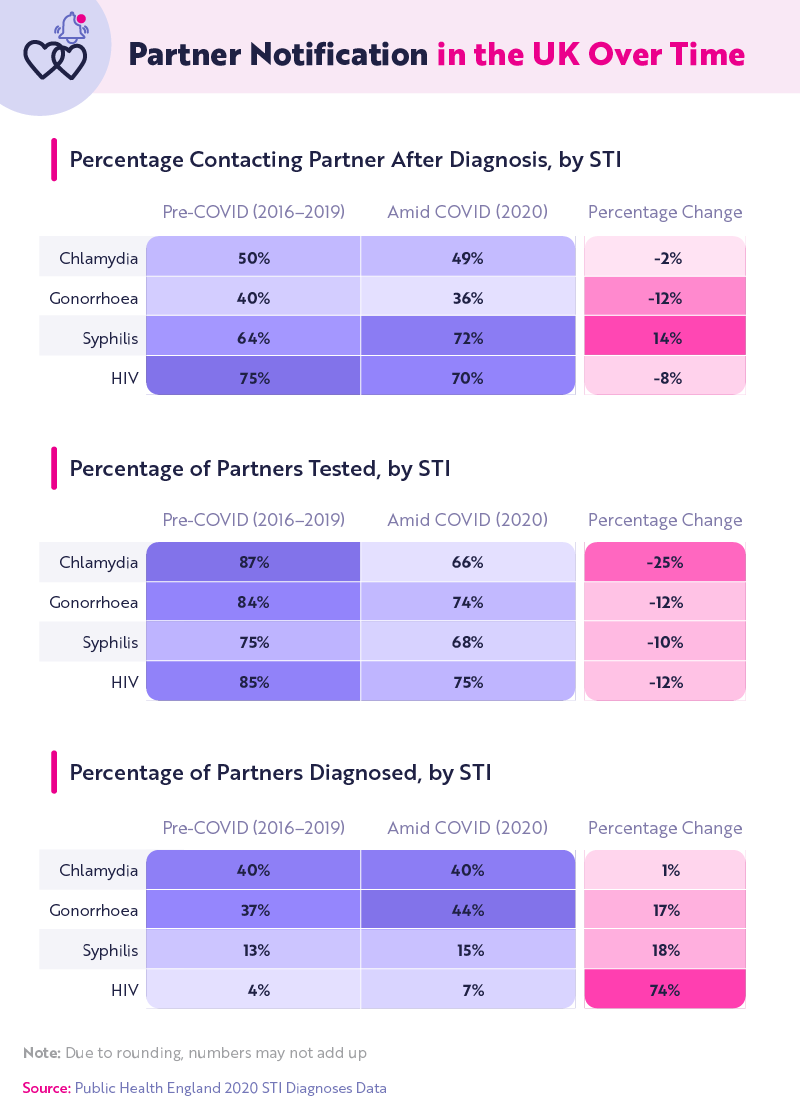
Partner notifications decreased for most STIs during COVID-19. Those diagnosed with syphilis were contacting their partners more during COVID, with partner notifications seeing a change of 14%. Fewer overall diagnosed cases of STIs during COVID could be due to fewer sexual encounters during lockdown or less testing and reporting. While there was an increase in STI tests and diagnoses after lockdown restrictions eased in June 2020, there were still fewer STI consultations, vaccinations, tests, diagnoses, and treatments than in the corresponding months of 2019.
Perhaps the most pertinent change is that people who were notified that their partner had an STI were less likely to get tested themselves during COVID-19. For instance, more than 87% of people who were told their partner had chlamydia between 2016 and 2019 then got tested themselves, compared to less than 66% of notified partners in 2020.
Interestingly, partners who did get tested had the same if not higher instance of a positive diagnosis for gonorrhoea, syphilis and HIV during COVID than before the pandemic. The difference was the starkest with gonorrhoea: Before the pandemic, less than 37% of partners tested positive for gonorrhoea, whereas during COVID, almost 44% of partners tested positive. This may suggest that partners were only willing to get tested during COVID if they felt they had a higher likelihood of having the disease—especially since it was harder to access health care during the pandemic, leaving many with unmet sexual health needs.
Reducing the Spread
The COVID-19 pandemic had a drastic effect on many people's health, including their sexual health. STI cases dropped dramatically during the year. This could be in large part because of nationwide lockdowns that kept people from engaging in sexual activities, but it could also be that fewer people were able to access the STI testing and treatment they needed.
Fortunately, improvements in telemedicine services and online consultations allowed people to continue getting access to the help they needed. The majority of respondents said they prefer accessing sexual health care online, which is where we come in. At Superdrug Online Doctor, we are here to help—operating discreetly to assist with your sexual health needs or questions. We offer testing, treatment, and so much more. Visit us today to gain peace of mind and to help reduce the transmission of STIs.
Methodology and Limitations
We surveyed 688 people in the UK and U.S. who contracted an STI in 2020. We queried them about their experiences with STI testing, diagnosis, and partner notification.
200 respondents were from the UK, and 488 respondents were from the U.S. Sixty-three percent of respondents were men, and 37% of respondents were women. Eight percent of respondents were Gen Zers, 59% of respondents were millennials, 25% were Gen Xers, and 8% were baby boomers or older.
To help ensure that all respondents took our survey seriously, they were required to identify and correctly answer an attention-check question.
The data are not weighted and are based on self-reporting. With self-reported data, there are limitations, such as the over- or underreporting of information as well as exaggerated numbers and answers.
Fair Use Statement
Part of helping eliminate the spread of STIs and HIV is being informed. We hope these findings were educational and informative. If you know someone who could benefit from our research, please feel free to share this study. However, we ask that you do so for noncommercial purposes only and include a link back to this article so that everyone can benefit from the findings in their entirety






