-
Men's Health
-
Women's Health
-
Sexual Health
-
Chronic
-
Travel
-
Book online for vaccinations for
travel and general health in one
of over 60 clinics nationwide
-
-
Wellbeing
-
Testing Services
-
Help & Contact
-
What Is Superdrug Online Doctor?
We're a service that helps you order treatments online from UK-registered doctors with free, discreet, to-your-door deliveries.
-
The STI Stigma Report: Let’s Talk About It
Over a million STIs are diagnosed around the world each year, and hundreds of thousands of people search their symptoms online in the UK on a regular basis, perhaps secretly searching for confirmation or remedies after a sexual encounter.
But apart from the obvious, what impact does contracting an STI have on people, and why is there still such a crippling stigma around them, when they are so common and treatable?
We wanted to explore the UK’s perceptions of STIs, and in particular how people talk about STIs to others - whether that be their doctor, friends, family, partner or even a first date. We also spoke to STI experts, psychologists, dating experts and those who have had STIs themselves, to gain their valuable insights and tips on how to talk clearly and openly about STIs and a diagnosis.
Who does the UK turn to for STI advice?
We conducted a survey of 2,000 sexually active adults and discovered that, understandably, the most trusted group of people to turn to was a doctor, with 75% saying they would feel comfortable speaking to a medical professional if they had an STI.
However, most don’t feel able to confide with anyone other than a professional, with 63% saying they wouldn’t feel comfortable going to their friends, 90% not wanting to speak to their parents or siblings, and almost 1 in 2 wouldn’t even speak to their long-term partner about it.
Insights from Dr Vanessa Apea, Sexual Health and HIV doctor
Dating with an STI
So if people won’t even talk to their long-term partner about an STI, what chances does a first date have? According to experts, it’s important to be up front about your STI status when dating, but according to our survey, people would rather discuss their ex-partner on a first date than their STI status.
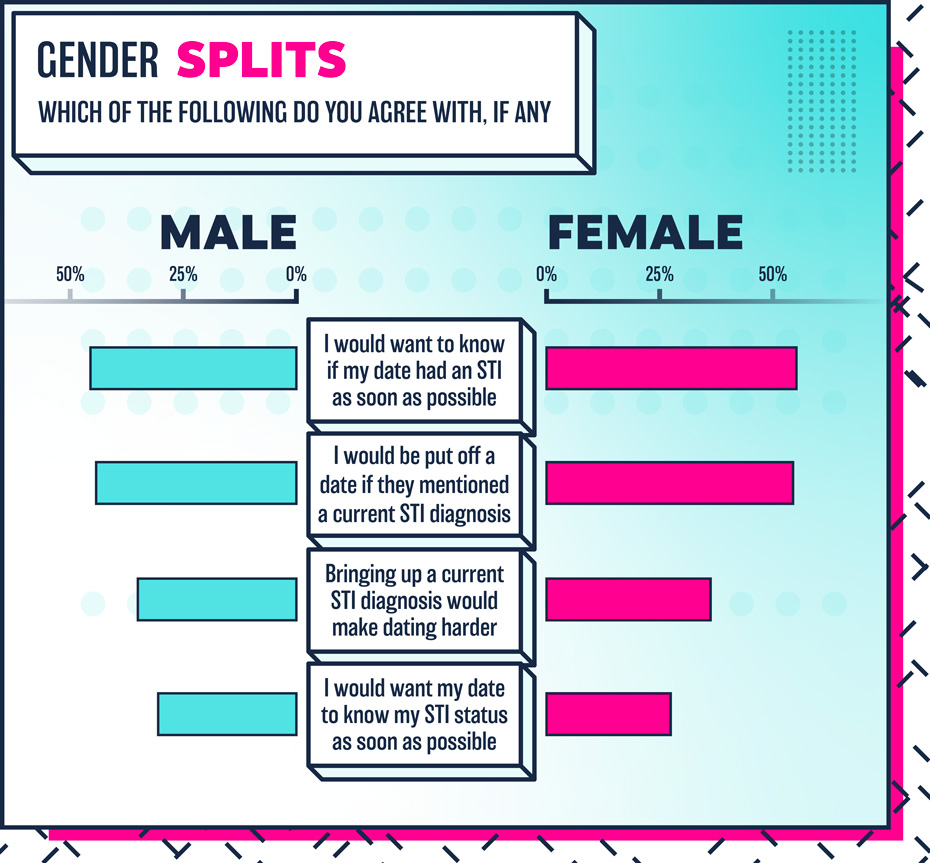
It may not be the most sexy of conversations, but it’s crucial to let a potential sexual partner know your situation and ensure safe measures are taken to prevent further infection. 72% said the topic of STI status and sexual compatibaility would be the least comfortable topic to discuss on a date for them, highlighting the issues many have in broaching the topic.
However, there seems to be a discrepancy here, with over half (51%) saying they’d want to know if their date had an STI, yet just 28% saying they’d tell their date if they had one. Clearly, the current shame and stigma around the conversation prevents people from being up front themselves, but it doesn’t stop the majority of people wanting to know anyway.
Our sexologist expert, Jess O’Reilly PhD, explained how you can potentially approach the topic if needed:
“Talking about testing and STIs can be intimidating because of stigma and a general unease around sex. But talking about sex ought not to be awkward. If you’re comfortable enough to get naked and rub your bodies against one another, hopefully you’ll also cultivate a connection that allows you to talk about your desires, needs, boundaries and expectations around safer sex - which includes STI testing.”
According to Jess, some ways to make the conversation easier are:
- Bring it up when you talk about condoms or birth control: Do you have a condom? Is there a brand you want to use? Let’s talk about birth control and STI testing.
- Use your own testing history to start the conversation: “When were you last tested? My last test was in April.”
- Suggest testing together: “I always go on this day. Want to join?”
- Focus on their health: “I care about your health and mine, so let’s talk about STIs and testing.”
- If you’re talking about overall health, make sexual health a part of the discussion: Talk about your most recent STI test the way you talk about other health check-ins (e.g. annual physical)
- Consider ordering STI tests that you can use at-home – it’s really easy!
While 51% said they’d want to know if their date had an STI, 14% of people say they would never tell their partner about their STI status and 18% said they would bring it up only just before having sex, highlighting the split between those who want to know and those who are willing to say.
The impact of an STI
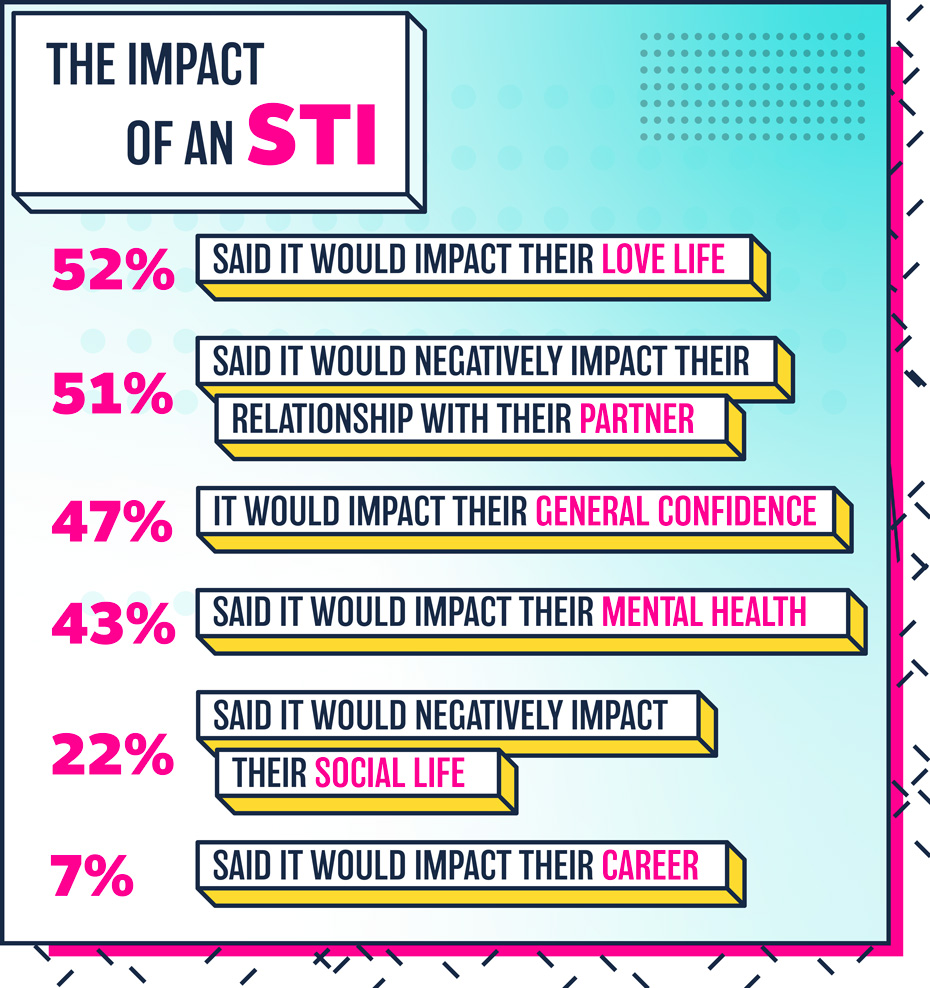
While the current conversation around STIs may be limited, what isn’t so contained is the impact an STI can have on people’s everyday lives, largely perhaps due to the stigma surrounding it, rather than the physical impact of the infection.
A huge 91% say that an STI diagnosis would negatively impact their mental health, relationships, social life, love life, general confidence or even their career.
 Audio insight from Kylie Yates - person with STI on - what impact it had on them
Audio insight from Kylie Yates - person with STI on - what impact it had on them
Education around STIs
Perhaps the reason for a lack of confidence to discuss STIs with people close to us, including our own partners or dates, and the large impact an STI can have in so many aspects of our lives, is that we just don’t know enough about them.
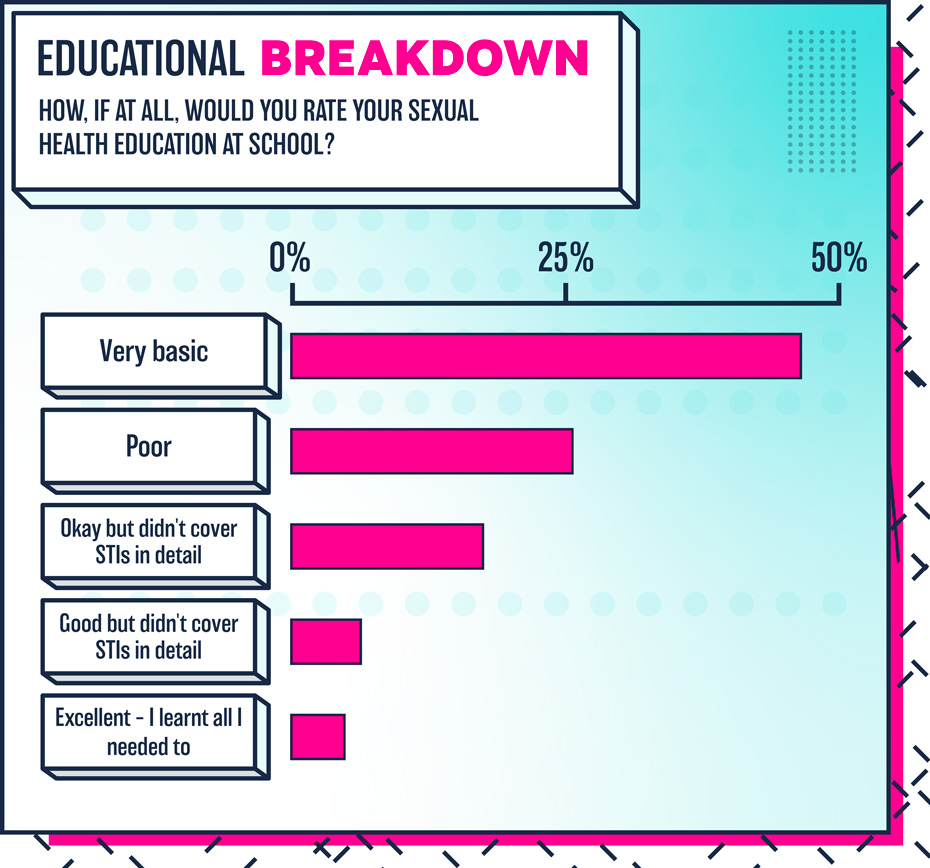
People are scared of the unknown, and are also understandably nervous about something that has for many years been portrayed as a scary, dirty or worrying thing to avoid at all costs. The fear of STIs has taken over, and this could be down to a lack of solid education on the topic, stemming back to our school days.
Incredibly, our study revealed that 72% said their sex education at school was very basic or poor, and just 4% said their sex education experience was “excellent.”
With hundreds of years of stigmatisation and poor education to overcome, it’s a tough task to change the way in which we’ve all learned to view and talk about STIs. From sex education posters in school, old government documentation, or even the way STIs have been weaponised and spoken about online through insults, it’s clearly an uphill battle to discuss STIs and get tested, despite how simple it can be. Here we can see how old sentiments and conversations around sex and STIs can be transformed for the better - slide down to transform the messaging…
Expert Tips for talking about STIs
Talking about sex and STIs can be tricky, especially with someone who you are, or planning to be, intimate with. We spoke to Julia Kotziamani, a love, sex and relationship expert and educator, as well as sexologist, Jess O’Reilly (PhD), who provided their top tips for talking to a partner about STIs.
- Start the conversation early
Start early on in the relationship (ideally before you are intimate) and normalise it being a topic you discuss openly. If it’s too late for that, then start asap. We are all grown ups and know that sex can cause infections so jumping in and being up front is the best option. To help with this you can talk openly with friends and normalise it for yourself before chatting to your partner.
- Get knowledgeable about STIs
On that, get knowledgeable! It’s so much easier to talk about things you know about, and knowing your own status is really important when getting comfortable with the topic. Following sex positive Instagram and TikTok accounts, reading the NHS website and other education platforms such as here on Superdrug Online Doctor can help you learn and make the conversation feel less alien for you.
- Be open and accepting
Be open with your partner, and also accepting. Being able to create a judgement free environment is a really positive place to start. Unless neither of you had any sexual contact prior, you both need to take responsibility for being tested, be honest about your pasts, and be able to hear things that may be a little challenging. A safe space without judgement can make the whole conversation a lot more comfortable.
- Remove the shame
Stigma can only exist where there is shame. And STI stigma is potentially very dangerous! You don’t have to treat STIs like a death sentence. They’re simply a risk associated with sexual activity. Especially since STIs can be either cured or treated — there is no shame in testing positive for one. But if you let shame hold you back from testing, you’re putting yourself at greater risk of transmitting an STI or dealing with the long term effects of leaving it untreated (e.g. infertility, pelvic pain, ectopic pregnancy). Realising that we can all get STIs even if we take precautions is a good place to start your own process of acceptance.
- Stay up to date with testing
Make sure you are up to date with your own tests and vaccinations. This means you can be totally honest about where you are. You could even use your own testing history to start the conversation.
- Remember the first time is the hardest
Know that the first time is the hardest! Once these conversations just become part of your dating life they become second nature. It will get easier and is such an important part of healthy dynamics and wellness. Conversations don’t have to be super heavy and serious… or even face to face. As long as you are communicating, that’s fine. Some people prefer to text if it’s a new or casual partner. It can be very chilled.
- Consider your partner’s discomfort in the topic
If a partner doesn’t want to talk about STIs and testing, don’t assume that it’s a red flag. Shame and stigma around sex make talking about sex challenging, so don’t assume that their discomfort talking about STIs is an indication that they don’t want to practice safer sex. They may simply be uncomfortable with the conversation itself, so ask them what you can do to put them at ease — it may be a matter of timing, language or location.
- Be prepared for their reaction
If you disclose a positive status, remember that their reaction is more about their own level of comfort and knowledge — it’s not about you. If they’re judgmental, it’s likely a matter of their own discomfort. It obviously isn’t your job to educate others, but you may find it helpful to provide info about transmission, management and treatment.
In Summary
Whether you’re single, dating, or in a relationship, STIs can be a conversation many aren’t ready to have, and our research shows it’s not a topic many want to have. However, with greater education, support and understanding, we can work together to ensure the stigma and shame associated with STIs are reduced, and open conversations can be had without an issue.
Regular testing is absolutely crucial to remain safe when sexually active, but testing from home is quick and easy. From chlamydia and gonorrhoea tests, to syphilis, herpes and HIV, you can view our range of STI home test kits here, and use the following 10% discount to make testing even easier: TESTME






